Gastroesophageal Reflux Disease (GERD)
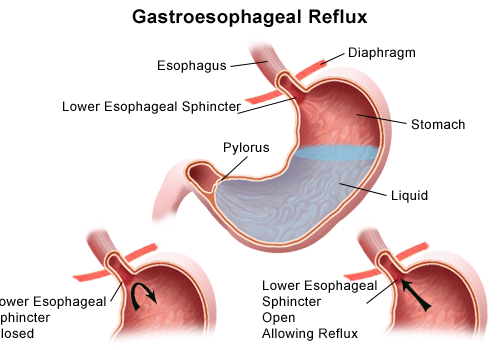 Gastroesophageal reflux disease (GERD) is defined as a condition that develops when the reflux of stomach contents causes troublesome symptoms and/or complications. Reflux of acid can be physiologic (usually no symptoms, typically occur postprandially, are short-lived, and rarely occur during sleep) Pathologic reflux is associated with symptoms or mucosal injury, often including nocturnal episodes and is what referred to as GERD.
Gastroesophageal reflux disease (GERD) is defined as a condition that develops when the reflux of stomach contents causes troublesome symptoms and/or complications. Reflux of acid can be physiologic (usually no symptoms, typically occur postprandially, are short-lived, and rarely occur during sleep) Pathologic reflux is associated with symptoms or mucosal injury, often including nocturnal episodes and is what referred to as GERD.
GERD is classified based on the appearance of the esophageal mucosa on upper endoscopy into the following:
- Erosive esophagitis is characterized by endoscopically visible breaks in the distal esophageal mucosa with or without troublesome symptoms of GERD.
- Nonerosive reflux disease or endoscopy negative reflux disease is characterized by the presence of troublesome symptoms of GERD without visible esophageal mucosal injury.
GERD can be with or without esophageal inflammation. Reflux esophagitis describes a subset of patients with symptoms of GERD who also have endoscopic or histopathologic evidence of esophageal inflammation. Reflux of acid from the stomach due to reduced LES tone, causing irritation and inflammation of the lower esophagus and the GEJ. Irritants that commonly get refluxed include alcohol, gastric acid.
Etiology and Risk factors for GERD:
- Risk factors: Smoke, Alcohol, Caffeine, Chocolate, Mint, Spicy food, Medications like (Calcium Channel Blocker, nitrates)
- CREST Syndrome can increase GERD (The E stand for Esophageal dysmotility, meaning no contract nor relax from fibrosis and atrophy of smooth muscle; lack of peristalsis of lower esophagus)
- Hiatal Hernias and Surgery for Achalasia are also common risk factors for GERD.
- Other causes: (CNS depressant, Hypothyroidism, Nasogastric intubation)
Symptoms and Clinical Presentation:
- Heart burn (mimic cardiac chest pain up to throat) usually post prandial
- Regurgitations: perception of flow of refluxed gastric content into the mouth or hypopharynx
- Dysphagia (if esophageal stricture develop as a result of healing process due to prolong erosive/ulceratie esophagitis of GERD) due to stricture.
- Odynophagia rare unless there is erosion causing esophageal ulcer.
- Epigastric pain → relieved with antacid
- Indigestion (dyspepsia)
- Asthma (adult onset); Chronic cough that wheeze (25% of chronic cough are GERD due to bronchospasm)
- Laryngitis
- Sore throat, bad metallic/bitter taste in mouth.
- Damage to enamel teeth (due to acid refluxed to mouth) with a bitter taste (acidic/metallic)
- Regurgitation especially when lying down hence night cough with wheezing!
Unusually Atypical GERD Symptoms:
- Atypical GERD symptoms also include restrosternal chest pain that can mimic angina, resolving either spontaneously or with antacids.
- Hypersalivation (due to acid),
- Globus sensation is the almost constant perception of a lump in the throat (irrespective of swallowing), which has been related to GERD in some studies. However, the role of esophageal reflux in globus is uncertain.
- Odynophagia is an unusual symptom of GERD but, when present, usually indicates an esophageal ulcer.
- Nausea is infrequently reported with GERD, but a diagnosis of GERD should be considered in patients with otherwise unexplained nausea.
Diagnosis of GERD (Reflux disease):
- Often clinical if have typical symptom and proceed treatment
- No Alarm symptoms (Sx) no need upper endoscopy
- PPI for 8 weeks twice a day (if still symptom positive → upper endoscopy)
- Symptoms of GERD with Alarm symptoms too (weight loss, anemia, GIB, recurrent vomit, dysphagia, odynophagia)
- Most accurate (24 hour pH monitor) rarely done unless equivocal presentation
- upper endoscopy indicated – Alarm Symptoms or 5-10 years of GERD to rule out barrett’s esophagus or post 8 week PPI persistent symptoms before upper endoscopy, because want to see if there is complication of GERD or other diagnosis for symptoms.
- Esophagitis (erosive esophagitis)
- Peptic strictures, Barrett’s esophagus, esophageal adenocarcinoma.
Complications:
- Mild Bleeding, Ulceration with stricture formation like Rings (from scarring) – symmetric circumferential stricturing (hence cause dysphagia to solid, not liquid) usually no weight loss unlike esophageal cancer where patient present with weight loss and has asymmetric structuring.
- Barrett Esophagus (late important complication) that can become (esophageal adenocarcinoma type)
- Bronchospasm (wheeze) and Aspiration Pneumonia
Treatment and Management:
- Initial PPI Treatment can be diagnostic and therapeutic (unless there is indication for upper endoscopy initially)
- Alarm symptoms: Weight loss, anemia, bloody stool, dysphagia.
- If patient have GERD and Alarm symptoms (need upper endoscopy, not empirical PPI)
- GERD without alarming symptoms
- Mild disease: Recommend starting with life style modification: lose weight, smaller meal, quit smoking, limit (Alochol, caffeine chocolate, mint, No eating 3 hour before sleep.
- If life style modification does not work, start PPI (95% patients have their symptoms controlled with this regimen)
- H2 inhibitors (cimetidine, ranitidine) – Mild intermittent symptoms when PPI not available. (H2 blocker have inferior result compared to PPI)
- Proton Pump Inhibitors (omeprazole, pantoprazole etc.) – persistent symptoms
- Surgery is indicated when there is no response to PPI or if patient have refractory side effects to PPI). The choice of surgical procedure are as follows
- Nissen fundoplication; LES suture to tighten it from allowing reflux; Heat or radiation of LES to cause scarring and hence stricture.
