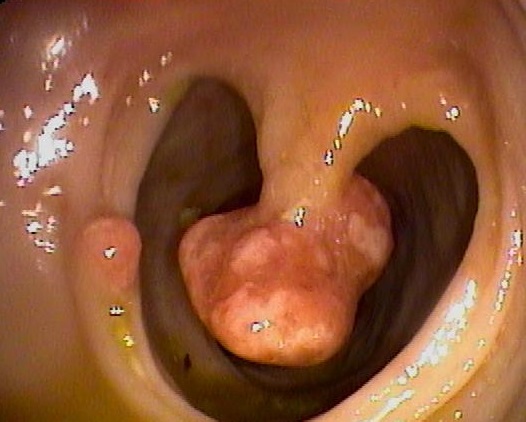
Colonic Polyps
A polyp is any protrusion or elevation of the intestinal surface into the lumen. A polyp can occur in esophagus, stomach, small intestine, gall bladder and Colon (most common). We will focus on colonic polyps since they have relevance in developing into colon cancer.
Types of Colonic Polyps
Colonic polyps can be categorized into 2 types: Neoplastic vs Non-neoplastic
Non-neoplastic Polyps (2 types)
- Non-neplastic polyps aris due to either abnormal maturation or inflammation.
- Inflammatory Polyps: Common in inflammatory bowel disease (Ulcerative Colitis, Chron’s Disease)
- inflammatory polyp do carry some risk of cancer as seen in patient with IBD, especially ulcerative colitis that have risk of developing colon cancer
- Non-inflammatory Polyps can be sub divided into
- Hyperplastic from mucosal proliferation which are very common and no further workup is necessary. This is the most common non-inflammatory polyps.
- Harmatomatous (Peutz jegher syndrome removed due to bleeding risk; Peutz Jegher Polyps)
Neoplastic Polyps (adenoma): ( 3 types)
- benign but has potential to be malignant adenocarcinoma
- Adenoma most commonly affect colon glandular cells, hence called adenomas (adenomatous polyps) – show epithelial dysplasia and hyperchromaticity < 1%.
- They start off benign but has potential to become malignant (invasion of submucosal stalk)
- The 3 types of neoplastic adenoma (polyps) are as follows.
- Tubular Adenomas: (75%): Pedunculated, Smaller, can be have malignant foci but less potential to be malignant compared to villous adenoma.
- Villous Adenomas: (10% less common): Sessile, Larger, highest potential to be malignant.
- Tubulo-villous Adenomas: (15%) variant that has characteristics intermediate of both
Prognostic Factors for risk of colon cancer
- Sessile villous polyps have more potential to be malignant as opposed to tubulous pedunculated polyps.
- Larger polyps more have more risk of malignant potential than smaller polyps
- The degree of dysplasia is also important prognostic factor of polyp turning cancer
- Negligible (< 1.5 cm); intermediate (5-2.5 cm); substantial (> 2.5 cm) polyps
Symptoms and Clinical Presentations
- Most adenomatous polyps are usually asymptomatic
- However, they may present with anemia due to occult blood loss.
- Villous adenoma can lead to loss of fluid, protein and electrolyte causing hypoproteinemia, hypokalemia.
Diagnosis of Colonic Polyps
- Diagnosis can only be made with colonoscopy.
- All patient at 50 years old require a colonoscopy screening.
- Those with family history of colon cancer will require more strict screening guidelines (see Endoscopy Screening)
Genetic Predispoition
- HNPCC (Hereditary Non-Polyposis Colorectal Cancer)

- This means don’t necessary need polyp to become cancerous. HNPCC is also known as Warthin Lynch Syndrome. It is a defective DNA Mismatch Repair gene (MLH1, MSH2) causing Microsatellite instability (MSI). Patient with HNPCC less commonly form polyps than FAPs. HNPCC are more commonly right sided. Tumors may be multiple and mucinous in histology. Precursors can be: Hyperplastic Polyps, none, Sessile serrated adenoma.
- FAP variants: (no screening recommendations)
- Gardner Syndrome: Autosomal dominant predisposition characterized by FAP plus Multiple osteomas, Congenital hypertrophy of retinal epithelium, fibromatosis (desmoids tumors), epidermal cyst
- Turcot Syndrome: is characterized by FAP plus CNS tumors like glioblastoma among others.
- Familial Adenomatous Polyposis: (FAP)
- Predispose mutation of a copy of APC gene on chromosome 5 (autosomal dominant)
- Develop 1000s (minimum 100 to diagnose FAP) of polyps and by age 40 will develop invasive carcinoma (colorectal cancer).
- Panproctocolectomy recommended (followed with ileo-rectal anastomosis)
- Harmatomatous (Non-inflammatory Non-neoplastic Polyps) 2 types we will go through
- Juvenile Polyps aka Retention Polyps (Autosomal Dominant)
- Common in children less than 5 years old
- Rectum is most common site
- If only one polyps called juvenile polyps. If multiple called Juvenile Polyposis Syndrome (JPS)
- Sporadic one polyps (No malignant potential); JP syndrome (increase risk of malignancy)
- Juvenile Polyps are also seen in PTEN mutation associated Syndromes: Cowden Syndrome and Dannayan-Ruvacalba-Riley Syndromes
- Peutz Jegher Polyps (Autosomal dominant) – no extra screening
- Also have sporadic and Syndromic forms like JPS.
- Multiple polyps in whole GIT but mainly in small intestine, colon.
- Juvenile Polyps aka Retention Polyps (Autosomal Dominant)
- (freckles like) Melanotic Pigmentations in mucocutaneous areas (Lip, Perioral, Face, Genitalia, Palms)
- See multiple harmatoartous polyps throughout small bowel and colon.
- Arborizing network of smooth muscles extending into the polyps and surrounds glands
- Glands are lined by non-dysplastic epithelium rich in goblet cells
- Yes Malignant potential in colon ( slightly higher than general population get colon cancer: 10% vs 6-8%) but such patients are at risk of developing carcinomas of pancreas, lung, breast, ovary, uterus.
What are types of Harmatoma Tumor Syndrome?
- Cowden Syndrome (also PTEN harmatoma tumor syndrome)
- Bannayan-Riley-Ruvalcaba syndrome (also PTEN harmatoma tumor syndrome)
- Proteus syndrome
- Proteus-like syndrome
- Juvenile Polyps Syndrome
- Peutiz Jegher Syndrome
What are PTEN hamartoma tumor syndrome?
This is a group of syndrome with PTEN mutation
- Cowden Syndrome
- Bannayan-Riley-Ruvalcaba syndrome
- Proteus syndrome
- Proteus-like syndrome
Management and Treatment of Colonic Polyps
Removal of colonic adenomas is important for minimizing cancer risk and mortality. Hence it is important to screen for polyps and remove them before cancer develops. We have already covered how colonoscopy are essential to screening for colonic polyps/cancer.
The removal of polyps called polypectomy is important in management of polyps. Many techniques are used during colonoscopy to remove polyps including:
Snare Excision, Biopsy forceps, Simple fulguration, including with argon plasma coagulation, Saline assisted endoscopic mucosal resection, Endoscopic submucosal dissection.
Snare excision is the most commonly used method for polypectomy of polyps >5 to 10 mm. Lesions less than 5 mm are removed with either biopsy forceps or by snare polypectomy.