Gastroenterologist South Florida Best Florida Gastroenterology Practice!
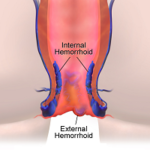
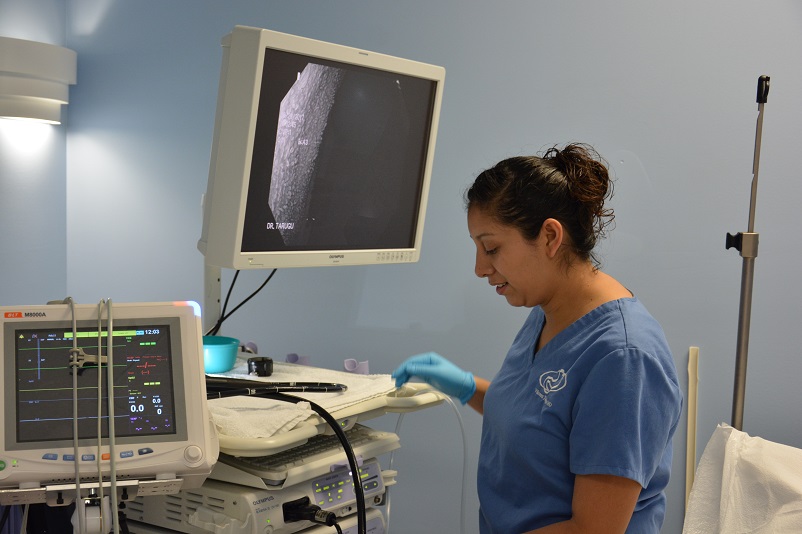
Dr. Vikram Tarugu, is a best-in-class, board certified gastroenterologist in South Florida. Specializing in the diagnosis and treatments of gastrointestinal tract conditions.
Dr. Tarugu is currently in private practice and has privileges at Raulerson hospital. He is also the CEO of Detox of South Florida. He is routinely rated as one of the best GI doctors and liver doctors in Florida. Patients through out the US have sought his expertise and seek his help when a second opinion is needed with difficult and chronic Gastro intestinal and liver diseases.
Dr. Tarugu provides services to patients in Okeechobee county, Treasure coast area, Port St. Lucie, Fort pierce, Sebastian, Vero beach, belle glade , Stuart , Arcadia,Sebring and Palm beach gardens, Fl.