Hepatitis is defined as the inflammation of the liver. There are many causes of inflammation of the liver, including infectious and non-infectious causes. They can be viral or non-viral like alcoholism, acetaminophen, autoimmune etc. The 4 most common cause of liver inflammation (hepatitis) include:
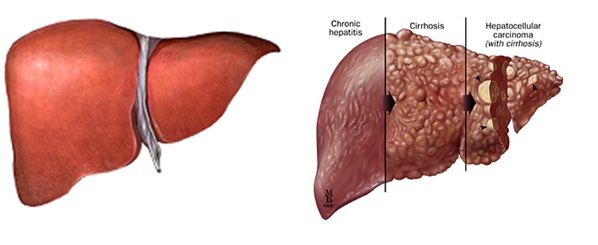
- Viral (Hepatitis, Adenovirus, CMV, EBV, HSV, Yellow fever). Acute infection means less than 6 months while chronic means more than 6 months. Most viral hepatitis do not have a chronic course, but hepatitis B and C have risk for becoming chronic and can cause cirrhosis and eventually heaptocellualr carcinoma (HCC).
- Alcoholic Hepatitis
- Medication induced (Acetaminophen, RIPE therapy for TB)
- Autoimmune Hepatitis
Viral Hepatitis
Table of Contents
- 1 Viral Hepatitis
- 1.1 Incubation Periods of Viral Hepatitis
- 1.2 Symptoms of Hepatitis A to E
- 1.3 Diagnosis of Hepatitis Infection
- 1.4 Diagnostic Workup for Hepatitis B
- 1.5 Diagnostic Workup for Hepatitis C
- 1.6 Vaccination and Treatment
- 1.7 Treatment and Management for Hepatitis C Infection
- 1.8 Treatment and Management of Hepatitis B Infection
- 2 Alcoholic Hepatitis
- 3 Autoimmune Hepatitis
Viral hepatitis cause by inflammation of the liver parenchyma usually due to hepatitis virus, others include CMV, EBV with destruction of hepatocytes from CD8+ cells.
Hepatitis A and E are transmitted via fecal-oral route by contaminated food and water. They are orally ingested and have an asymptomatic incubation period of several weeks (2-6 weeks). They cause symptomatic disease for several days to weeks, but do not cause chronic infection and do not lead to either cirrhosis or hepatocellular carcinoma.
Hepatitis B, C, and D are transmitted typically by parenteral route. They can be transmitted perinatally or through sexual contact, blood transfusion, needle stick, and needle sharing in IV drug users (IVDU). Hepatitis B and C can lead to a chronic infection and have the risk of causing cirrhosis and hepatocellular carcinoma. Hepatitis C is the most common disease leading to the need for liver transplantation in the United States. Hepatitis D when co-infected with Hepatitis B can often lead to fulminant hepatitis and cause liver failure.
Hepatitis G has been identified in a small number of patients through screening of the blood supply but no clinically relevant disease has been identified.
Incubation Periods of Viral Hepatitis
The incubation period for Hepatitis A and E is around 1 month. Whereas for Hepatitis B and C is about 3 months on average. Hepatitis D has an incubation period of about 1-2 months.
Symptoms of Hepatitis A to E
All hepatitis can present with jaundice, dark urine, light colored stool, fatigue/malaise, weight loss, right upper quadrant pain and hepatosplenomegaly. Hence you cannot differentiate the type of hepatitis based on symptoms alone. In fact drug induced hepatitis like isoniazid, alcoholic hepatitis can also have similar symptoms) Of note: Hepatitis B and C can both give serum-sickness like syndrome (joint pain, rash vasculitis and glomerular nephritis). Cryoglubulinemia can also occur in hepatitis C and B. Hepatitis E present with severe symptoms of hepatitis in pregnant women.
Diagnosis of Hepatitis Infection
The diagnosis of hepatitis rely not only on the history and clinical presentation. Serum markers plays a key role in diagnosis. All patient should be tested for the following
- Antibodies, viral antigens when relevant, AST/ALT, alkaline phosphatase, Total bilirubin and direct bilirubin. The most important workup for hepatitis virus infection is Hepatitis B (HBV) and Hepatitis C (HCV) infection.
- In severe disease (PT and albumin may also be abnormal)
- Viral hepatitis: elevated ALT > AST
- Alcoholic hepatitis: elevated AST > ALT more than 2.
Diagnostic Workup for Hepatitis B
- The initial workup for Hepatitis B
- Most of the time in chronic hepatitis B: HBsAg is positive (by definition > 6 month post infection)
- When HBsAg is positive, Anti-HBs antibody is always negative (they are busy neutralizing antigen)
- When HBsAg is negative, Anti-HBs antibody is positive (seroconversion) is most cases.
- HBeAg in an indication of active replication, Anti-HBe antibody is usually negative.
- Acute HBV infection:
- 3 possible phase (early phase, window phase, recovery phase) see table below
- Sequence of elevation: HBV DNA → HBsAg → (HBeAg, ALT elevation, Symptoms if present)
- Chronic HBV infection:
- Persistence of HBsAg for more than six months, presence of IgG
- HBeAg and serum HBV DNA measure to determine if the patient should be considered for antiviral therapy. ALT may be normal or mild/moderate elevated.
- ALT is measure to monitor progression of the disease whereas HBV DNA is measured to predict chronic HBV progression.
Diagnostic Workup for Hepatitis C
- The initial diagnosis for patient presenting with acute hepatitis symptoms (regardless of type) is:
- Relevant antibodies (both Hepatitis B and Hepatitis C) and screen for HIV (due to common risk).
- HCV RNA and relevant markers: AST/ALT, INR, Bilirubin, Alkaline phosphatase.
- AST/ALT can be in the 1000s or sometimes normal
- HCV-RNA Positive:
- Anti-HCV antibody negative: Acute Hepatitis C (need to check Ab in 12 months if Ab negative for seroconversion)
- Anti-HCV antibody Positive: Can be acute or chronic need to check past 6 months if HCV RNA or antibody.
- Yes past 6 month was negative for HCV RNA or Ab test implies Acute HCV infection
- No past 6 month was also positive already: Then you need to ask if there is recent high risk exposure: Yes (Probable acute HCV infection); No (Probable Chronic HCV infection)
- HCV-RNA Negative
- Anti-HCV antibody negative (acute infection unlikely) – most people fall here.
- Anti-HCV antibody positive: recheck HCV RNA after 12 weeks to recheck
- Positive HCV RNA → acute hepatitis C.
- Negative HCV RNA → prior hepatitis c infection that has resolved.
- All possible Positive Acute HCV infection need to be re-evaluated in 12 weeks for clearance or seroconversion if antibody was negative initially.
- The diagnosis for chronic hepatitis C is the same as acute hepatitis: HCV RNA and Anti-HCV antibody.
- Positive HCV RNA (PCR) for > 6 months post exposure is diagnostic for chronic HCV infection.
- AST and ALT are also tested but has limited value (30% have normal ALT). Only 25% have ALT > 2x the normal limit.
Vaccination and Treatment
There is only vaccine for Hepatitis A and Hepatitis B. All newborn are vaccinated with hepatitis A and B. Hepatitis A is also given to those travelling to countries that may have contaminated food and water, chronic liver disease, and those with high risk sex behaviors. Treatment is only relevant for Hepatitis B and C.
Chronic Hepatitis B has many effective medications. Hepatitis C on the other hand, for many years have limited treatment options. As of 2014, there has been many new HCV medications approved by FDA. In the past, only Ribavirin, (interferon) IFN are used. We will look more at the treatments for Hepatitis B and Hepatitis C below.
Treatment and Management for Hepatitis C Infection
HCV is on the cutting-edge of medicine where treatment of Hepatitis C can be as effective as up to 99%. FDA recommend Harvoni™ (Sofosbuvir/Ledipasvir) co-medication for treatment of Hepatitis C positive patients.
Acute Hepatitis C
- Acute hepatitis diagnosed before chronic infection can be managed by several approaches.
- Watch and wait for 12 weeks for spontaneous resolution:
- If does not resolves after 12 weeks, treatment initiation
- If infection resolves, no treatment but follow up necessary because a single negative HCV RNA is not enough to declare spontaneous clearance. In addition, patients should be counseled to decrease risk factors and abstain from alcohol, hepatotoxic drugs like Tylenol.
- Treatment depends on the financial status
- No insurance coverage patient are usually given IFN-alpha for 24 week if HCV genotype-1, 12 weeks for other genotypes.
- In the presence of HIV co-infection: Add Ribovarin (RBV) to the treatment regimen.
- Insurance coverage for DAA (Direct-acting anti-viral): Treatment is like chronic hepatitis C
Chronic Hepatitis C
- IFN-free regimens are available. Ideal regimen depends on several parameters
- Previous treatment, Other medication used
- Genotype of virus (genotype-1 most common in USA)
- Fibrosis presence and extend of liver damage, Renal impairment presence.
- First line: Harvoni™ (Sofosbuvir/Ledipasvir) co-medication in most situations
- Treatment naïve: with or without cirrhosis: Harvoni for 12 weeks
- Treatment naive: no cirrhosis, RNA < 6 million IU/ml: Harvoni™ for 8 weeks
- If drug is working, HCV RNA should be undetectable by (4-12 weeks)
- Goal of antiviral therapy in patients with chronic hepatitis C virus (HCV) is to eradicate HCV RNA, which is predicted by attainment of a sustained virologic response (SVR), defined as an undetectable RNA level 12 weeks following the completion of therapy.
Treatment and Management of Hepatitis B Infection
- Hepatitis B can be treated with the following medication. There is no increase efficacy if combined together.
- (IFN-α, Lamivudine,Telbivudine, Adefovir, Entecavir, Tenofovir)
- Lamivudine (high resistance, rarely used unless with HIV, potent control of Hepatitis B
- Adefovir (less resistance, but least potent antiviral med)
- Telbivudine, Entecavir – both better than Lamivudine potency and low resistance but side effects Telbivudine (peripheral neuropathy and myopathy)
- Tenofovir (first line for treatment naïve or treatment resisitant patients), next better maybe (Entecavir)
- Renal Failure (Entecavir > Tenofovir); Compensated Cirrhosis (Tenofovir > Entecavir)
- Decompensated Cirrhosis (No IFN-α, All types ok)
Alcoholic Hepatitis
Alcoholic inflammation of the liver parenchyma usually due to heavy alcohol consumption. The cause of alcoholics hepatitis has to do with heavy drinking (binge) or a continuum from fatty liver requiring long term sustained consumption. Other risk factors include (Reye syndrome, CO poisoning, Kwashiokor-fatty liver due to decrease synthesis of ApoB to coat VLDL.
Pathogenesis:
- Fatty Yellow Greasy liver (steatosis) is due to Alcoholic induced disturbance of fat metabolism,
- High amount of cytoplasmic NADH formed by Alcohol DH and Acetaldehyde Dehydrogenase increase NADH which cause hypoglycemia (inhibit gluconeogenesis) and increase DHAP conversion to Glycerol-3- phosphate to form Gylcerol and fatty acid.
- Alcohol also decrease beta oxidation reaction in the mitochondria.
- Intracellular accumulation of fat from faulty metabolism, with lipid vacuoles displace the nucleus – macrovesicular change – reversible
- Eventual Fibrosis around central vein that is irreversible.
- Course: Hepatic steatosis leads to alcohol hepatitis and from reversible to irreversible transition to alcohol cirrhosis.
Lab Diagnosis:
- Elevated ALT, Elevated AST. The pattern of elevation tell different causes of hepatitis
- Elevation of AST>ALT with greater than 2: 1 ratio implies alcoholic hepatitis.
- Binge drinking cause elevated GGTP
Progression and Complications
- Each acute episode has 20% risk of death
- Repeated episode increase risk of cirrhosis to HCC
Autoimmune Hepatitis
Autoimmune attack of the liver with unknown cause but associated with Coombs positive hemolytic anemia, thyroiditis, ITP
Clinical presentations
- Signs of liver inflammation (elevated AST/ALT) with mild elevate/normal Alkaline phosphatase
Diagnosis
- Initial = ANA +ve and anti smooth muscles test, Serum protein electrophoresis (SPEP) show hypergammaglobulinemia.
- Very high elevation of AST/ALT.
- Specific Diagnostic test include: liver-kidney microsomal antibodies, ↑IgG, anti-smooth muscle antibody.
- Most Accurate test for diagnosis of autoimmune hepatitis is liver biopsy
Treatment and Management
- Prednisone is commonly used, but for those dependent on steroid can be wean off steroid using other immunosuppressants: Azathioprine
